Among chest wall deformities in children, Pectus Carinatum is the second most common after Pectus Excavatum. Unlike the inward depression of funnel chest, Pectus Carinatum is characterized by a forward protrusion of the sternum, resembling the breastbone of a chicken or pigeon. Many parents notice their child's chest "sticking out" and worry about both appearance and health, yet they are often unsure how to intervene effectively. With advances in non‑invasive orthotic technology, a corrective approach based on external compression—the Pectus Carinatum Brace (chest wall compression brace)—is now offering a non‑surgical treatment option for an increasing number of children. This article provides a detailed overview of the principles and clinical outcomes of brace therapy for pediatric pectus carinatum.
Pectus carinatum, commonly known as pigeon chest, is a chest wall deformity characterized by forward protrusion of the sternum. It is the second most common chest wall deformity in children, with an estimated incidence of approximately 0.1% and a male‑to‑female ratio of about 4:1. Most cases become noticeable after age 5 or 6, and the deformity often becomes more pronounced during the adolescent growth spurt.
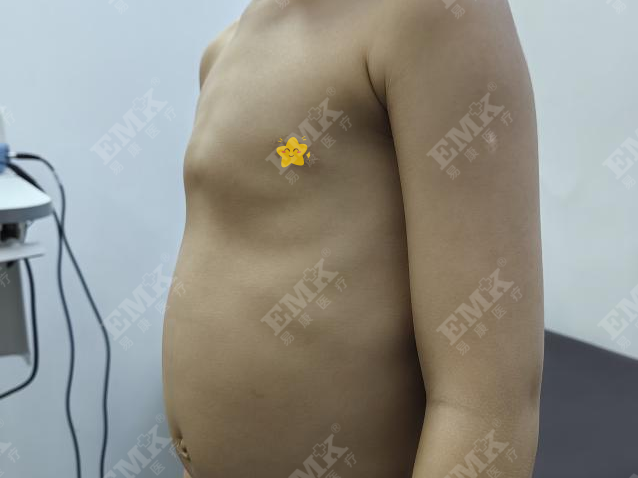
Unlike Pectus Excavatum, pectus carinatum increases the anteroposterior diameter of the chest; the thoracic volume is not necessarily reduced, but severe cases can still affect cardiopulmonary function. Because of its prominent appearance, children with pectus carinatum are more likely to experience psychological stress and social challenges during school age and adolescence.
The principle of brace therapy for pectus carinatum is similar to orthodontic treatment for teeth—using sustained, gentle external pressure to guide bone remodeling during a child's growth and development.
A pectus carinatum brace is a custom‑fitted chest compression orthosis, typically made from high‑strength, lightweight materials that conform to the anterior and posterior chest. When worn, the brace applies sustained, controllable pressure to the protruding sternum via a front pressure pad, while a rear support panel provides counter‑pressure, creating a stable mechanical system.
This external pressure acts on the protruding sternum and costal cartilages, inhibiting further forward growth while guiding the costal cartilages and sternum to develop toward a normal contour. As the child grows, the bones gradually shift toward a normal shape under the combined effects of pressure inhibition and growth guidance.
In children and adolescents, the chest wall is not yet fully ossified, and the costal cartilages retain good elasticity and plasticity. Regular, consistent use of the brace during key growth periods provides external intervention that can:
Inhibit excessive growth at the protruding area
Guide the costal cartilages to develop with a normal curvature
Promote overall improvement of chest contour
This is a gradual process, typically requiring consistent wear for months to 1–2 years, depending on the child's age, severity of the deformity, and compliance.
As a non‑invasive treatment, the pectus carinatum brace has been adopted in several pediatric hospitals in China. Below are summarized results from published clinical studies and hospital experience for parental reference.
A study from Shandong Provincial Hospital retrospectively analyzed children treated with a pectus carinatum brace. The study included 38 patients aged 4–16 years (32 males, 6 females). The mean sternal protrusion height before treatment was 19.6 mm.
Results:
Mean sternal protrusion height after treatment decreased to 7.2 mm
Mean correction rate: 63.3%
92.1% of patients achieved "satisfactory" or "good" improvement
No severe adverse reactions were reported
The study showed that younger age was associated with better outcomes. Children aged 4–8 years achieved better results than those aged 9–16 years, highlighting the importance of early intervention.
Based on clinical experience from multiple hospitals:
| Age Group | Observations |
|---|---|
| 3–8 years | Good chest wall flexibility and cooperation; ideal improvement with relatively shorter treatment duration |
| 9–12 years | Still in a growth phase; stable improvement achievable but requires longer wear time |
| 13 years and older | Skeletal maturation reduces correction potential, but improvement is still possible for mild to moderate deformities |
Compared with surgical correction, brace therapy is generally far less expensive, does not require hospitalization, and leaves no incisions—offering families an alternative treatment option.
Based on clinical experience, brace therapy may be considered for:
Younger children with good skeletal plasticity
Patients with mild to moderate pectus carinatum
Children whose families prefer to avoid surgery
Patients with recurrence or suboptimal results after surgery who need adjunctive correction
Children experiencing psychological distress due to appearance and seeking non‑surgical improvement
Coagulation disorders (e.g., hemophilia)
Severe skin diseases
Allergy to brace materials
Skeletal disorders (e.g., osteogenesis imperfecta)
Severe underlying cardiopulmonary disease requiring priority management
Based on clinical protocols:
Initial fitting: A physician or orthotist adjusts the brace according to the child's chest contour, ensuring accurate pressure placement and appropriate force
Adaptation period: The first 1–2 weeks are for adaptation; wear time can be gradually increased from a few hours per day to full‑day wear
Consistent wear: Typically recommended for 12–20 hours per day, adjusted according to physician guidance and patient tolerance
Regular follow‑up: Re‑evaluation every 3–6 months to assess progress; brace adjustment or replacement as needed
Clinical data indicate a low incidence of side effects with brace therapy, which may include:
Local skin redness and mild discomfort
Sensation of restricted movement during initial wear
Skin friction irritation
These effects are usually mild and resolve with adjustment of wear technique, use of protective padding, or after the adaptation period. Caregivers should monitor closely and consult a physician if significant discomfort occurs.
Before starting treatment, have your child evaluated by a specialist (pediatric thoracic surgeon or orthotist) to determine suitability
Consistent, regular wear is essential—intermittent use will compromise outcomes
Schedule a follow‑up evaluation after 3–6 months of consistent use to assess progress
If no significant improvement is seen after 6–12 months, consult a thoracic surgeon to discuss next steps
As the child grows, the brace may need to be replaced periodically (typically every 6–12 months) to maintain proper fit and pressure effectiveness
The availability of the pectus carinatum brace provides a non‑surgical corrective option for some children. Current clinical observations show that for younger children with mild to moderate deformities, consistent brace wear can achieve satisfactory improvement, and some children may avoid surgery altogether.
Even in cases where brace therapy does not achieve the desired result, surgery can still be considered at a later time; early brace use does not typically interfere with surgical timing and may help slow the progression of the deformity, creating more favorable conditions for subsequent treatment.
With advances in 3D scanning and 3D printing technology, custom‑fitted pectus carinatum braces can now be designed based on each child's chest contour, achieving more precise pressure distribution and better wearing comfort. Digital design and manufacturing make braces lighter, more breathable, and more discreet—improving patient compliance.
A Note from EMK:
If you notice a forward protrusion of your child's chest, we recommend seeking evaluation from a pediatric thoracic surgeon or pediatrician. Early intervention and scientifically guided correction are essential steps in helping your child achieve a healthy chest contour.
Disclaimer: This article is for educational purposes only and does not constitute medical advice. If you have concerns about your child's chest development, please consult a qualified healthcare professional.
Contact: KAM
Phone: +86 1365 2921 391
Tel: +86 1365 2921 391
Email: 1752119111@qq.com
Add: Orthosis Customization Center, 6th Floor, Rehabilitation Building, Guangdong Maternal and Child Health Hospital
We chat
