Among chest wall deformities in children, Pectus Excavatum is one of the most common. Many parents notice a "dent" in their child's chest that caves inward like a funnel, raising concerns about both appearance and potential health impacts. With advances in medical technology, a non‑surgical treatment using negative pressure—the vacuum bell—now offers a new option for some young patients. This article provides a detailed overview of the principles and clinical observations of vacuum bell therapy for pediatric Pectus Excavatum.
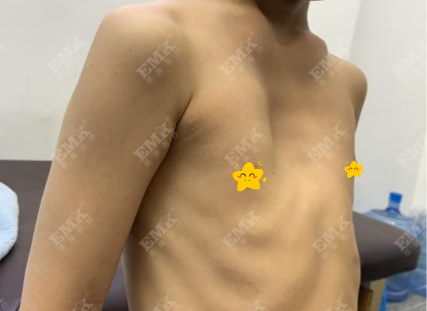
Pectus excavatum is a chest wall deformity in which the sternum and adjacent ribs curve inward and backward, creating a funnel‑shaped depression. It is a common congenital chest wall abnormality in children, with an estimated incidence of 0.1%–0.4%. The condition is 3–5 times more common in males than in females. Although the deformity may be present at birth, it often goes unnoticed until months or even years later, when it becomes more apparent as the child grows.
The principle of vacuum bell therapy is to use physical negative pressure to gradually elevate the sunken chest wall.
A vacuum bell is a device that conforms to the chest contour to create a sealed chamber. It is placed over the depressed area and sealed against the skin. By evacuating the air between the device and the chest wall, negative pressure is generated. This suction force gently lifts the depressed sternum outward—effectively applying an upward pulling force from the outside.
Users can adjust the suction force according to the instructions and their tolerance, raising the depressed area to a level close to the normal chest contour.
In children and adolescents, the chest wall is not yet fully ossified, and the costal cartilages retain good elasticity and plasticity. Regular, consistent use of the vacuum bell during growth can help guide the costal cartilages and sternum to remodel in a more normal direction, gradually improving the depression. This is a gradual process, typically requiring continuous use for months to years.
As a non‑invasive treatment, the vacuum bell has been adopted in several pediatric hospitals in China. Below are summarized results from published clinical studies for parental reference.
A study from the Children's Hospital of Chongqing Medical University retrospectively analyzed 100 young children (≤6 years old) with pectus excavatum treated with a vacuum bell between 2019 and 2023. Results showed:
Improvement was observed in 99 of 100 patients (99.0% improvement rate), with 52.0% showing marked improvement.
The average sternal depression depth decreased from 9.71 mm before treatment to 4.97 mm after treatment.
The study found no significant correlation between treatment outcomes and sex, type of pectus excavatum (symmetric vs. asymmetric), or severity (mild, moderate, severe). When broken down by age:
| Age Group | Number of Patients | Improvement Rate | Marked Improvement |
|---|---|---|---|
| 0–3 years | 57 | 100% | 49.12% |
| 3–6 years | 43 | 97.67% | 55.81% |
Other clinical observations have shown improvement rates of approximately 80% in children aged 1–8 years and 70% in adolescents aged 9–18 years, with younger children generally achieving better results than older children and adolescents.
Youngest patient: A 6‑month‑old infant with a pronounced chest depression and recurrent pneumonia was treated with a vacuum bell. The pre‑treatment sternal depression depth was 7.6 mm, with a Haller index of 3.15. After two years of treatment, the depression depth decreased to 3.4 mm, and the Haller index dropped to 2.5.
Experience at Children's Hospital of Zhejiang University: Since introducing this technique in 2016, hundreds of children have received vacuum bell therapy. Some patients show noticeable improvement after four months of use; the full treatment course typically lasts 2–3 years.
Compared with surgical correction, vacuum bell therapy is generally less expensive and can be performed at home, offering families an alternative treatment option.
Based on clinical experience, vacuum bell therapy may be considered for:
Children whose families prefer to avoid surgery
Younger children who do not yet meet surgical criteria
Patients with mild to moderate pectus excavatum
Patients with recurrent or residual deformity after Ravitch or Nuss surgery
Children with acquired pectus excavatum after cardiac surgery who are at high risk for Nuss procedure due to retrosternal adhesions
Coagulation disorders (e.g., hemophilia)
Severe skin diseases
Silicone allergy
Skeletal disorders (e.g., osteogenesis imperfecta)
Coexisting cardiopulmonary conditions (e.g., aortic aneurysm)
According to clinical protocols:
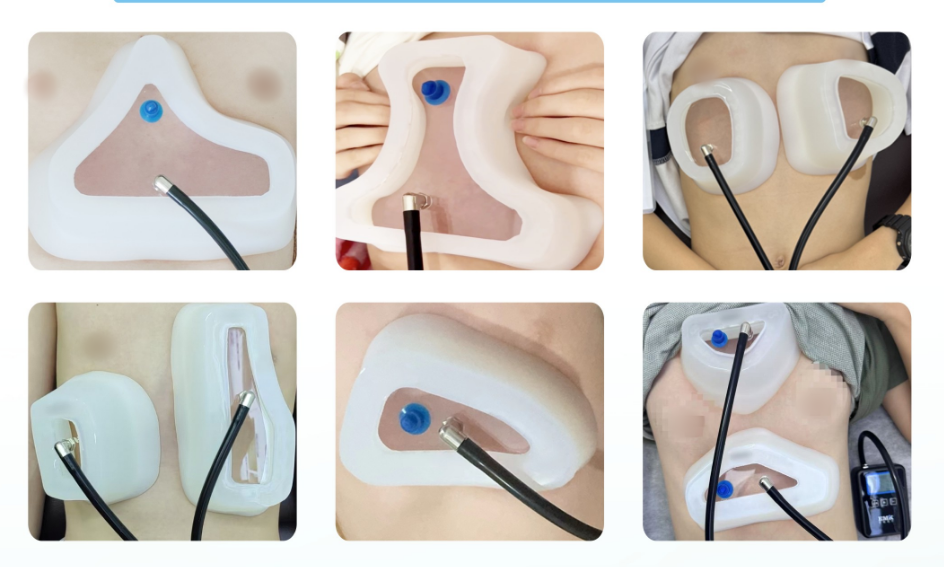
Position the vacuum bell over the depressed area, ensuring a good seal against the skin.
Evacuate air to generate negative pressure, lifting the depressed sternum toward a normal contour.
Each session is typically 30 minutes or longer, and it is generally recommended to use the device twice daily.
Suction strength and duration may be adjusted based on the child's tolerance and response.
Because young children are the primary users, caregivers should closely monitor the child's reaction during use and discontinue or adjust treatment if discomfort occurs.
Clinical data indicate an overall side effect rate of approximately 8.0%, which may include:
Local bruising or swelling of the chest skin
Local discomfort
Temporary numbness
These effects are usually mild and resolve after temporarily discontinuing use or adjusting suction strength and duration. Side effects are less common and generally milder in children under 10 years of age.
Before starting treatment, have your child evaluated by a specialist (pediatric thoracic surgeon) to determine suitability.
Schedule a follow‑up evaluation after three months of consistent use to assess progress.
If no significant improvement is seen after 3–6 months, consult a thoracic surgeon to discuss next steps.
The availability of vacuum bell therapy provides a non‑surgical option for some young children with pectus excavatum. Current evidence suggests it may help some patients avoid surgery altogether. Even in cases where vacuum bell therapy does not achieve the desired correction, proceeding with Nuss surgery remains an option; early use of the vacuum bell does not typically interfere with surgical timing and may even slow the progression of the deformity.
With advances in 3D printing technology, custom‑fitted vacuum bells can now be designed based on each patient's chest contour, further improving fit and treatment efficacy.
A Note from EMK:
If you notice a sunken appearance in your child's chest, we recommend seeking evaluation from a pediatric thoracic surgeon or pediatrician. Early intervention and scientifically guided correction are essential steps in safeguarding your child's health and well‑being.
Disclaimer: This article is for educational purposes only and does not constitute medical advice. If you have concerns about your child's chest development, please consult a qualified healthcare professional.
Contact: KAM
Phone: +86 1365 2921 391
Tel: +86 1365 2921 391
Email: 1752119111@qq.com
Add: Orthosis Customization Center, 6th Floor, Rehabilitation Building, Guangdong Maternal and Child Health Hospital
We chat
