Key Takeaways: Pectus Excavatum is a common congenital chest wall deformity characterized by posterior depression of the mid-to-lower sternum. It affects approximately 1 in 300–400 children, with a male-to-female ratio of about 4:1. This article provides a clear, evidence-based overview of pectus excavatum—its definition, clinical impact, and underlying causes—empowering readers to recognize early signs and seek timely intervention.
Pectus excavatum (PE), also known as funnel chest, is a congenital deformity of the anterior chest wall caused by posterior displacement of the sternum and the 3rd to 7th ribs or costal cartilages. Key features include:
Onset: Signs may appear in infancy and become more noticeable after age 3. During adolescence, rapid skeletal growth can deepen the depression.
Appearance: Common postural changes include forward-sloping shoulders, forward head posture, a hunched back, and a protruding abdomen. The deepest point is typically at the xiphoid process.
Types: PE is classified into symmetrical (most common, central depression), asymmetrical, high‑type, and broad‑type variants.
Differential Diagnosis: Unlike rickets—caused by vitamin D deficiency and accompanied by systemic symptoms like irritability, sweating, and rachitic rosary—PE is an isolated structural deformity without systemic bone abnormalities.
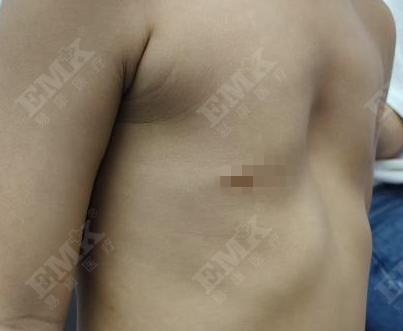
The severity of symptoms correlates with the degree of depression. PE affects both physical health and psychological well‑being.
Cardiopulmonary Impairment (Primary Risk): A depressed sternum compresses the heart and lungs, displacing the heart, reducing cardiac efficiency, and restricting lung expansion. This leads to chest pain, shortness of breath, poor exercise tolerance, and palpitations. Severe cases may progress to heart failure and increased respiratory infections, creating a vicious cycle of compression, infection, and functional decline.
Growth and Development (Critical for Children): Reduced thoracic volume hinders cardiopulmonary development. Abdominal compression may cause poor appetite, indigestion, and malnutrition, resulting in underweight status and delayed growth—especially concerning during key developmental years.
Secondary Deformities: Patients often adopt compensatory postures, leading to scoliosis or kyphosis, which further distort the chest and may cause back pain or, rarely, spinal cord compression.
Associated Conditions: Severe PE may coexist with pulmonary hypoplasia, Marfan syndrome, or asthma. Muscle weakness and skeletal instability can increase susceptibility to other thoracic conditions.
The visible chest deformity often triggers psychological distress, particularly in adolescents. Common effects include:
Low self‑esteem, anxiety, and sensitivity about appearance
Avoidance of activities that expose the chest (e.g., swimming, gym class)
Social withdrawal and introversion
Long‑term impacts on academic performance, career choices, and quality of life
Although less visible, these psychological consequences can be just as debilitating as physical symptoms and require equal attention.
While the exact cause is not fully understood, research points to a combination of congenital, genetic, and acquired factors.
Most evidence suggests that PE results from abnormal fusion of the sternum and costal cartilages during embryonic development. Overgrowth of the lower costal cartilages and ribs displaces the sternum inward. Additionally, a short substernal portion of the diaphragm may pull the sternum posteriorly, exacerbating the deformity. These changes originate in fetal life, become apparent after birth, and may worsen with age.
PE has a strong hereditary component, with approximately 40% of patients reporting a positive family history. Inheritance patterns include autosomal dominant, autosomal recessive, and X‑linked transmission.
Genetic studies have implicated mutations in genes encoding connective tissue proteins, such as FBN1 and COL2A1, which may lead to costal cartilage dysplasia. Individuals with a family history face a significantly higher risk, and males are more frequently affected.
Acquired Diseases: Severe rickets (vitamin D/calcium deficiency) can disrupt normal bone development. Chronic respiratory conditions like asthma increase negative intrathoracic pressure during inspiration, potentially pulling the sternum inward over time.
Connective Tissue Disorders: Syndromes such as Marfan syndrome and Ehlers‑Danlos syndrome are frequently associated with PE.
Iatrogenic and Traumatic Causes: Chest wall depression may occur after neonatal cystic adenomatoid malformation resection (due to loss of structural support) or following extensive chest wall trauma with unstable healing—both linked to weakened thoracic structure, abnormal mechanical forces, or altered intrathoracic pressure.
Pectus excavatum is a common congenital chest wall deformity that can significantly impact cardiopulmonary function, physical development, and psychological health. Its causes are multifactorial, involving congenital anomalies, genetic predisposition, and acquired factors. Early recognition, evaluation, and intervention are essential for optimal outcomes.
If you or a family member notice a sunken chest, shortness of breath with activity, or postural abnormalities, consult a thoracic surgeon promptly. Diagnosis typically involves chest X‑ray, CT scan (to calculate the Haller index), and electrocardiography.
Based on severity, treatment options range from conservative management (Pectus Excavatum Vacuum Bell therapy) to surgical correction. Early intervention can effectively restore chest contour, improve cardiopulmonary function, reduce psychological distress, and help patients return to a normal, active life.
Contact: KAM
Phone: +86 1365 2921 391
Tel: +86 1365 2921 391
Email: 1752119111@qq.com
Add: Orthosis Customization Center, 6th Floor, Rehabilitation Building, Guangdong Maternal and Child Health Hospital
We chat
